Technology Pipeline
- Home
- What We Do
- Technology Pipeline
- Diabetes Related Dry Mouth
Let’s Chat
Please feel free to contact us. We will get back to you with 1-2 business days.

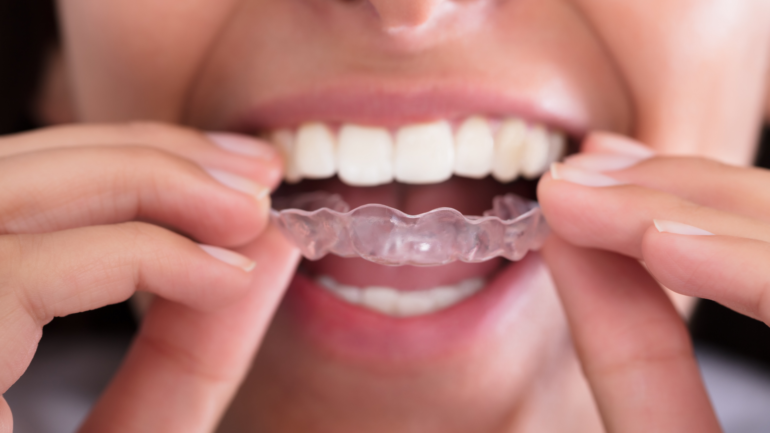

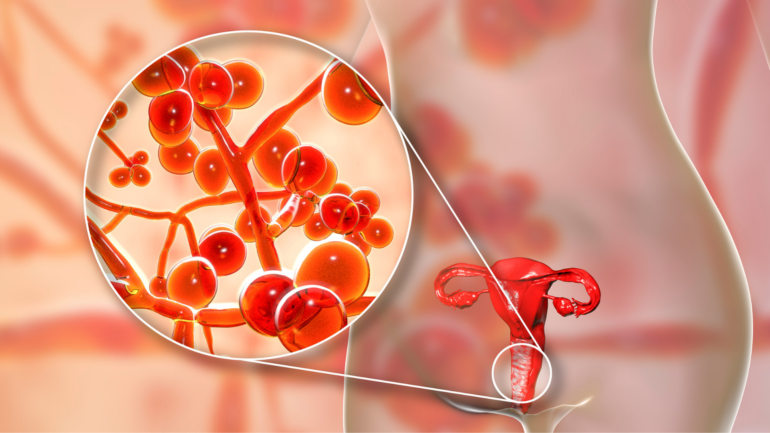

Diabetes-Related Dry Mouth
Diabetes has long been associated with oral manifestations. Many research reports throughout the world have sought to clarify the importance of diabetes as a risk factor for oral conditions. Several studies have shown correlations between diabetes and periodontal disease. An increased incidence of dental caries in association with poorly controlled diabetes has also been reported. Xerostomia (dry mouth) has been reported to be a common complaint of patients with diabetes. Without adequate saliva production, both hard and soft tissues of the mouth can be severely damaged and become more susceptible to infection. Xerostomia is an uncomfortable condition that can lead to dental cavities, changes in the oral mucosa, e.g., candidal infections, impairment of taste and burning mouth.
Supporting Salivary Gland Function
Diabetes mellitus has been consistently reported to alter salivary gland function through the same mechanisms as in cardiovascular or renal diabetic complications: autonomic neuropathies, microvascular changes, underlined by oxidative stress. The influence of dysfunctional autonomic nervous system in non-insulin-dependent diabetes patients was indicated by correlation between stimulated saliva secretion and different heart conditions. The condition is not inconsequential and impacts the quality of life.
Our Research
Xerostomia (dry mouth) has been reported to be a common complaint of patients with diabetes, without adequate saliva production, both hard and soft tissues of the mouth can be severely damaged and become more susceptible to infections. An IRB approved, double blind, cross over, placebo-controlled study was conducted in the Division of Endocrinology and Metabolism, Saint Louis University. In this study, a novel Hyaluronic Acid solution was tested for treatment of dry mouth and its tolerability in type-2 diabetes patients with symptomatic oral dryness. The data obtained from the just concluded study is being analyzed.